
15 May Bridging Healthcare Inequality: What India Can Learn from Thailand’s Universal Coverage Model
Healthcare is not just a social good; it is an economic imperative. The World Health Organization shows that a 10-year increase in average life expectancy at birth is associated with an increase in economic growth of about 0.3–0.4% annually. Countries with stronger health systems benefit from higher labour productivity, reduced absenteeism, and improved long-term GDP growth. Yet, India continues to underinvest in a sector that directly shapes both human capital and economic resilience.
Public healthcare is the state’s promise to protect citizens’ health. Government spending on clinics, hospitals, and prevention not only treats illness but keeps society productive. While some emerging economies have successfully institutionalised equitable access, others, like India, continue to face structural bottlenecks that limit outcomes despite growth.
India’s Healthcare System
India presents a striking paradox: it is a global hub for advanced medical procedures and medical tourism, yet a significant portion of its population lacks access to affordable and quality healthcare. Globally, richer countries typically invest around 10–12% of GDP in health, but India lags behind. According to the 2024 Economic Survey, India’s total health expenditure was just 3.8% of GDP in FY2021–22. (By comparison, OECD countries average 9.3%.)
Fig 1: Current Health Expenditure (% of GDP) of India and the World
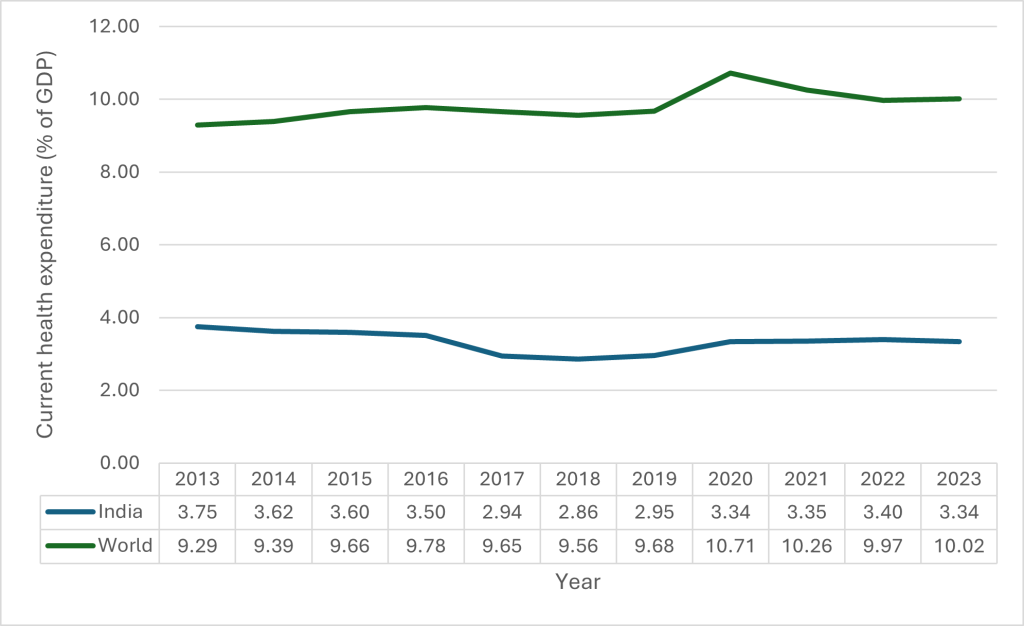
Source: The World Bank data
Interpretation: India’s health expenditure has remained persistently low at around 2.8%–3.7% of GDP between 2013–2023, compared to the global average of 9%–10%, reflecting a structural underinvestment in healthcare. While there was a slight rise during COVID-19 (2020), the increase was temporary, and spending stabilized again at 3.3%, indicating the absence of long-term fiscal prioritization. This gap is largely driven by:

Thailand’s Healthcare System
Thailand, a developing country like India, has become a global model for universal health coverage (UHC).
Fig 2: Current Health Expenditure (% of GDP) of India, Thailand and the World
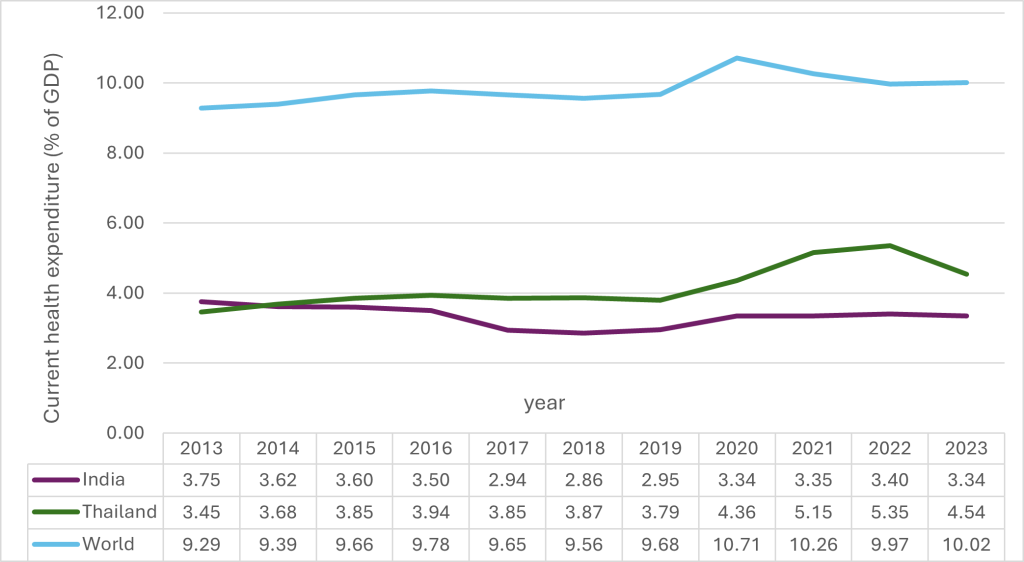
Source: The World Bank data
Interpretation: Thailand’s health expenditure has steadily increased from 3.4% in 2013 to over 5% in recent years, reflecting sustained fiscal commitment. Unlike India’s flat trend, Thailand demonstrates a clear upward trajectory, indicating long-term prioritization rather than reactive spending.

According to the World Bank Data, these combined interventions have led to strong health outcomes, with Thailand achieving higher life expectancy (77 vs 72 years in India) and lower infant mortality (6–8 vs 25 per 1,000), supported by reduced out-of-pocket spending (10% vs 44%) and higher public investment. This demonstrates that strategic system design, not just higher spending, drives results, as Thailand’s emphasis on primary care, efficient financing, and well-sequenced reforms has translated into better population health and stronger financial protection.

Conclusion
India’s healthcare challenge is no longer just about access; it is about building a system that delivers consistent, equitable outcomes at scale. Thailand demonstrates that even with limited resources, well-sequenced reforms, strong institutions, and clear policy prioritization can transform health systems.
Looking ahead, India’s demographic and economic trajectory will increasingly depend on the health of its workforce. As the country aspires toward becoming a $5 trillion economy, healthcare must shift from being treated as a welfare expense to a core pillar of economic strategy. The opportunity is clear: with the right structural reforms, India can transition from fragmented delivery to a resilient, productivity-enhancing healthcare system.
Blog by Samyuktha Purusothaman Nair,
Research Analyst, Frost & Sullivan Institute




